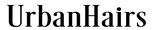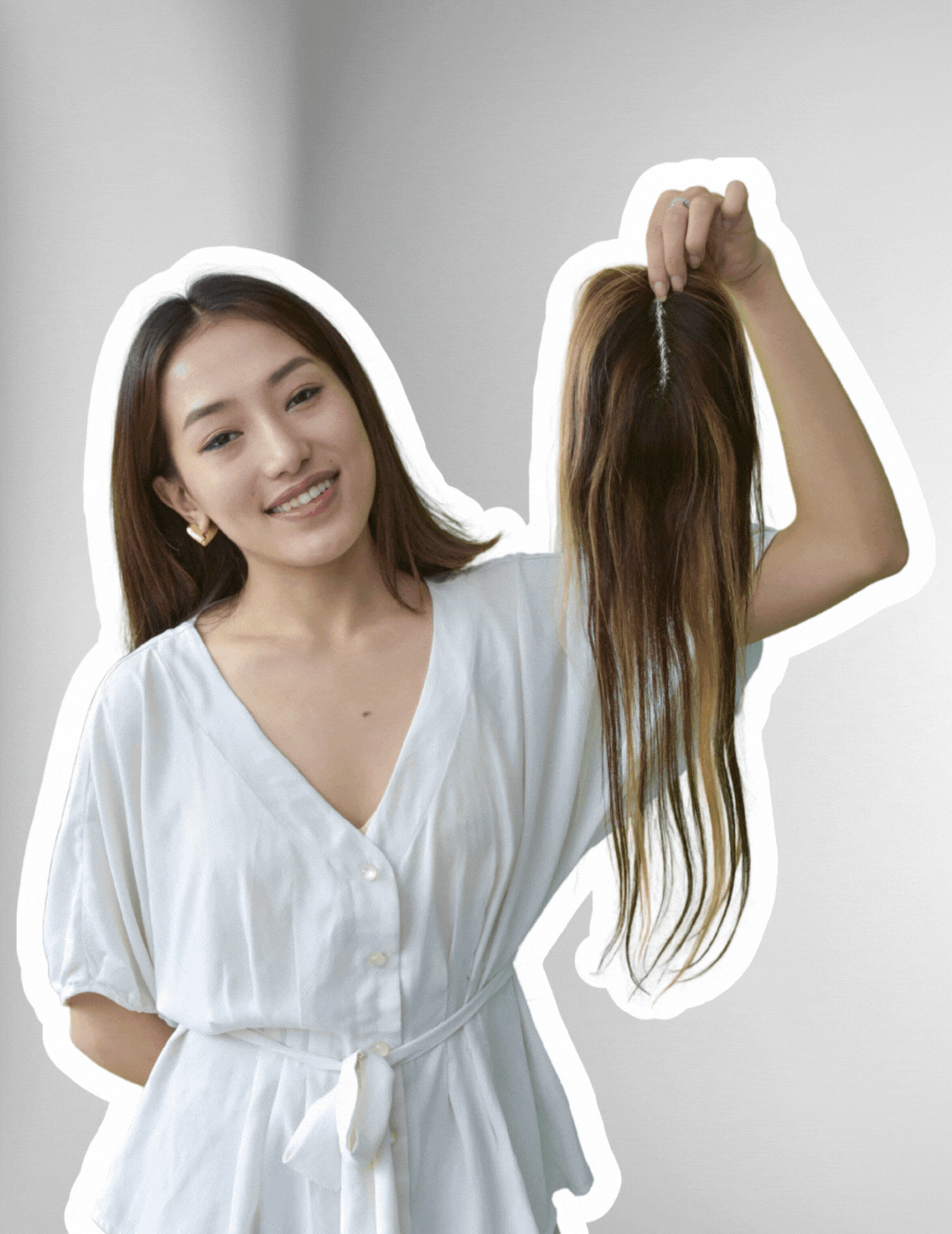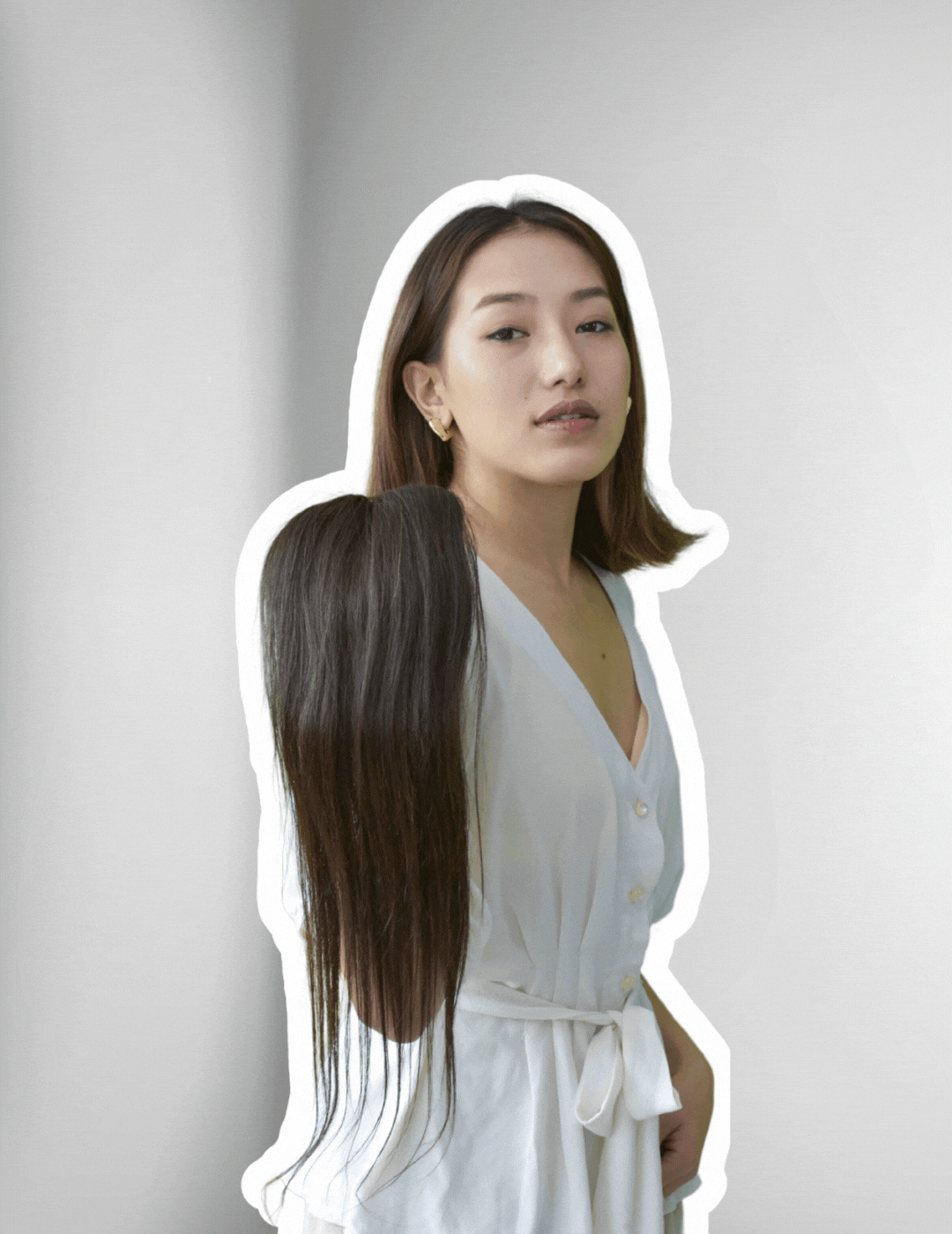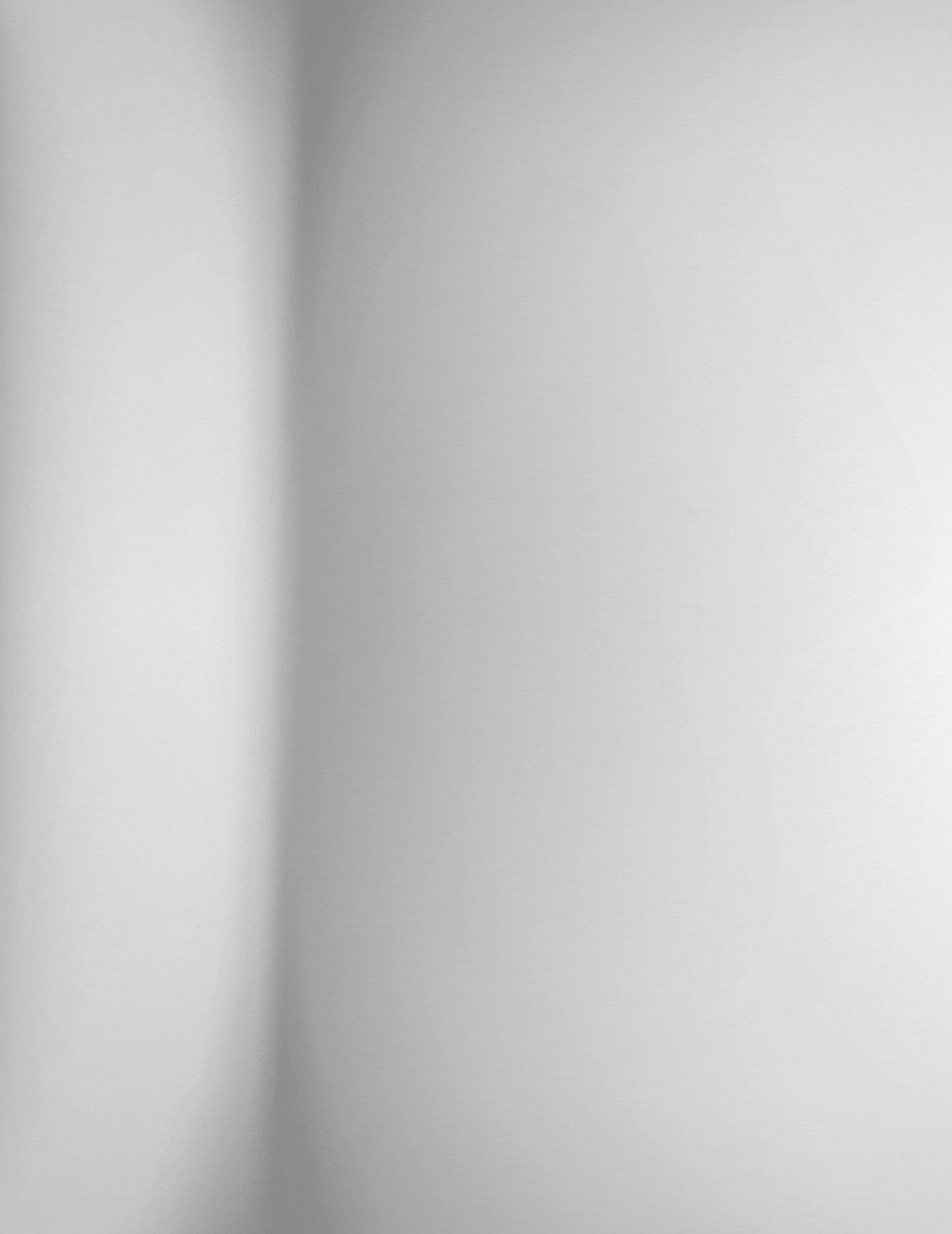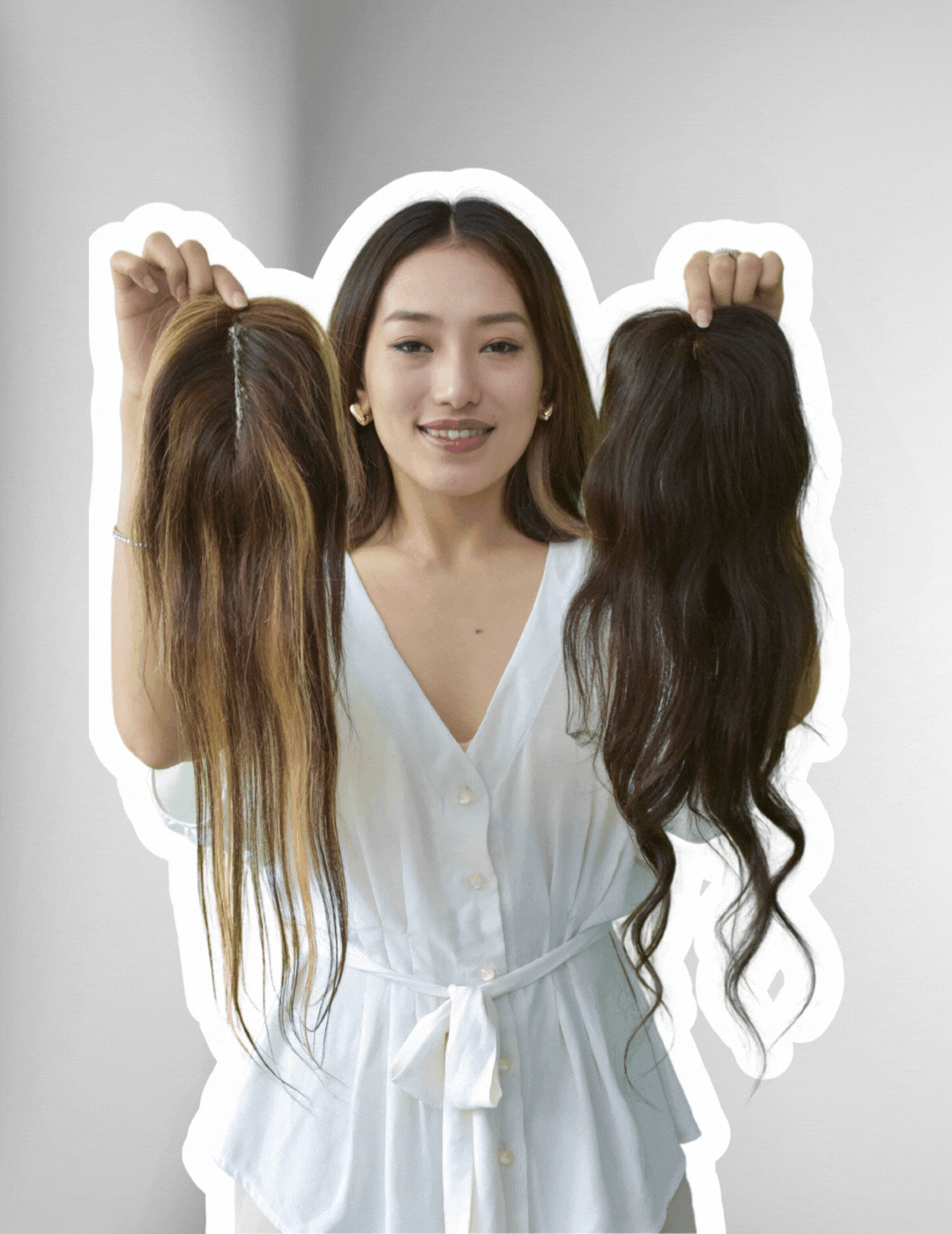Shop by Category
Shop the Look

Quick view
Korean Bangs | 100% Original Human Hair | Easy to use & Fix with Clips
-
Regular price
-
Rs. 1,199.00
-
Regular price
-
Rs. 2,999.00
-
Sale price
-
Rs. 1,199.00
Korean Bangs | 100% Original Human Hair | Easy to use & Fix with Clips
- Regular price
-
Rs. 1,199.00 - Regular price
-
Rs. 2,999.00 - Sale price
-
Rs. 1,199.00
Quick view
Ear to Ear Volumizer
-
Regular price
-
From
Rs. 4,999.00
-
Regular price
-
Rs. 10,000.00
-
Sale price
-
From
Rs. 4,999.00
Ear to Ear Volumizer
- Regular price
-
From
Rs. 4,999.00 - Regular price
-
Rs. 10,000.00 - Sale price
-
From
Rs. 4,999.00
Korean Bangs | 100% Original Human Hair | Easy to use & Fix with Clips




Korean Bangs | 100% Original Human Hair | Easy to use & Fix with Clips
- Regular price
-
Rs. 1,199.00 - Regular price
-
Rs. 2,999.00 - Sale price
-
Rs. 1,199.00
Ear to Ear Volumizer




Ear to Ear Volumizer
- Regular price
-
From
Rs. 4,999.00 - Regular price
-
Rs. 10,000.00 - Sale price
-
From
Rs. 4,999.00
Example product title
Vendor:
Vendor
Example product title
- Regular price
-
Rs. 19.99 - Regular price
-
- Sale price
-
Rs. 19.99
Lookbook

Quick view
Messy Bun Scrunchie | 100% Human Hair
-
Regular price
-
From
Rs. 1,299.00
-
Regular price
-
Rs. 2,199.00
-
Sale price
-
From
Rs. 1,299.00
Messy Bun Scrunchie | 100% Human Hair
- Regular price
-
From
Rs. 1,299.00 - Regular price
-
Rs. 2,199.00 - Sale price
-
From
Rs. 1,299.00
Quick view
Ear to Ear Volumizer
-
Regular price
-
From
Rs. 4,999.00
-
Regular price
-
Rs. 10,000.00
-
Sale price
-
From
Rs. 4,999.00
Ear to Ear Volumizer
- Regular price
-
From
Rs. 4,999.00 - Regular price
-
Rs. 10,000.00 - Sale price
-
From
Rs. 4,999.00
URban hairs SALONs
Collaboration Salons
Guarantees
Before & After